Dr. Lowenstein: Hi and welcome to the Headache 360 podcast. I am your host, Dr. Adam Lowenstein. We have a fantastic repeat guest today, Dr. Hossein Ansari, who is the head of the headache clinic at University of California, San Diego. This is our second in hopefully a series with Dr. Ansari, but you can refer to our first podcast with him for his outstandingly extensive degrees and education. Actually, so let me say again, Dr. Ansari, thanks for joining us.
Dr. Ansari: Thank you very much. Exactly what you were saying, thank you for working with me again. Hopefully this series of podcasts we can continue, because I believe it’s very important for education of the patients with headache and particularly migraine.
Dr. Lowenstein: Yeah. We’ve been getting a lot of great feedback, and actually your previous podcast is so far the most listened to one that we’ve had, the most downloaded, so thanks for that. I just wanted to say, which we haven’t talked about, but just looking online, your reviews are outstanding. It’s pretty rare, because when people come to me for migraine surgery, they’re usually complaining about their previous care, but just so many people fabulous doctor and very professional and he listens to all of my concerns. I guess if everybody was as good as a physician as you seem to be reviewed as, I think we’d have a lot better situation with migraines in general.
Dr. Ansari: Thank you very much. Actually it’s interesting you telling me, because I never actually look at my reviews online at all because that’s kind of giving me bias or also when you see one of 100 patients is not happy, they write something. I don’t want to even look at them.
Dr. Lowenstein: Now I hear you. It’s nice to see the good stuff. It hurts when-
Dr. Ansari: It really hurts, you know?
Dr. Lowenstein: You very rarely see the bad stuff.
Dr. Ansari: You know that you’re really working hard to help the patient, and one patient that, oh, okay.
Dr. Lowenstein: Right.
Dr. Ansari: So, that’s funny. But I’m glad [inaudible 00:02:49].
Dr. Lowenstein: But both of us seem to have a very high general level of reviews, so that’s great. What we’re going to talk about today is medications, right?
Dr. Ansari: Yes, yes. We decide to talk about the medication because that’s one of the biggest question that you always ask. Let’s start with this. When I go to different conferences, meeting or lectures here and there, one thing that they always they ask me, “What is your to go medication for migraine? What do you use for this?” This question doesn’t have answer, because we don’t have any to go medication for migraine. Each patient with headache and migraine is different. Again, I’m emphasizing here the difference between headache and migraine. Today we are talking just about the migraine. So, we know the migraine could be both over diagnosed and under diagnosed. That is very important to know. But again, that’s totally different podcast that we can use one hour to kind of go over.
Dr. Ansari: But let’s assume the patient has diagnosis of what we call migraine. One thing that we need to do before we start somebody on medication for migraine, to make sure patient’s headache and migraine is a pure migraine. There is no other big comorbidity that we need to fix or address before jump to the medication. One of the main reason that the medication treatment fail in the migraine because of probably lack of the time for most of the physician when the physician see the patient with migraine, they prescribe medication right away now looking at the entire picture. So, that is very important. Lifestyle, lifestyle change and patient’s basically other comorbidities play important role in term of considering what we need to know and even what medication we need to prescribe, because sometime when we prescribe medication for migraine, we basically use side effect of the medication as a benefit for that particular patient.
Dr. Ansari: Say, for example, patient with migraine also had anxiety and depression, which we know anxiety, depression is big comorbidity with migraine, about 60-70% of the patient with migraine also have comorbid anxiety and/or depression. So, for a particular patient, it’s very reasonable to use one of those antidepressants which FD approve for migraine to kill two bird with one stone. Right? That is-
Dr. Lowenstein: So, can I just ask, I have two questions real quick. This may be out of both of our per views, but do you think that the… what comes first, the chicken or the egg? The depression predates the migraines, or people become anxious and depressed because they have pain?
Dr. Ansari: I think both, because actually there’s a lot of studies on, again, this is whole separate podcast.
Dr. Lowenstein: Yeah, yeah, yeah, yeah.
Dr. Ansari: But one thing that’s very obvious, I mean, everybody can have common sense, if you have a lot of headache, you will be depressed. Right?
Dr. Lowenstein: Right, sure.
Dr. Ansari: If you have headache and you cannot go and do your daily activity or your hobby or something, you will be sad. Then that negative cycle continues, that is for sure. But also it has been shown that the patient had history or basically the predisposition for depression and anxiety used to get more migraine.
Dr. Lowenstein: Interesting.
Dr. Ansari: Because both is happening. But a very, very, very common comorbidity.
Dr. Lowenstein: And then I just want to get to something that you may be getting to eventually, but until recently, there weren’t really any medications for migraines. The point of the medication that were used were that we found that the medications also helped migraines despite what they were supposed to originally be for, and that’s why they were used. Is that a fair statement?
Dr. Ansari: Yes, exactly. We didn’t have a [inaudible 00:07:00] to talk about that when you’re talking about the different classes of the migraine, preventive treatment which is available. We will talk about that.
Dr. Lowenstein: Okay. Sorry to interrupt you then. Keep on going.
Dr. Ansari: Sure, yeah. My emphasis is in lifestyle. So, make sure patient does not have any important factor in his or her lifestyle that can trigger the migraine. For example, if you have a patient with a migraine who is he or she drinking a lot of diet Coke or two or three diet Cokes a day. We know any artificial sweetener is the biggest enemy for migraines.
Dr. Lowenstein: Wow.
Dr. Ansari: So, if the patient keep drinking that whatever Coke, diet tea or diet artificial stuff, so that’s it, that patient basically putting the fuel flaring the migraine. So, no matter what medication you give, the chance that that patient responds is low, so you need to make sure what is the patient’s diet, what he or she eats. All of this is important factor, as important as medication, if it’s not less.
Dr. Lowenstein: Interesting, okay.
Dr. Ansari: That’s why actually some other really, really good colleague in headache medicine, all they focus is in lifestyle, diet, and those parts. We have some headache doctor that their basically specialty or sub specialty is in this part. It’s very, very important. A patient with migraine should have regular, for example, exercise. You recommend the patient with migraine do 30 to 60 minutes of moderate intensity exercise five times a week. That is treatment that is as important as taking the medication.
Dr. Lowenstein: Interesting, okay.
Dr. Ansari: You cannot basically separate this lifestyle and activity from medication. But again, talking about the activity and what is good versus what is bad, that’s another podcast.
Dr. Lowenstein: Yeah, right, right. Sure. We’ve got a lot of podcasts to do.
Dr. Ansari: Yeah, I think so.
Dr. Lowenstein: All right.
Dr. Ansari: Now let’s go back to our treatment of the migraine. Now we are considering that we have the patient with migraine. If you are migraine, you add just all of the lifestyle, you know all of the potential trigger, and you want to give the medication. Medication for migraine we divide to two classes. One is called abortive or acute medication, which I am going to call abortive from now on, and the second is preventive or prophylactic medication, which I’m going to call preventive in this podcast.
Dr. Lowenstein: Okay.
Dr. Ansari: So, we have abortive versus preventive. What is that mean? Abortive treatment is the medication that the patient needs to take when he or she is going to get the migraine headache. Sooner you take is better. That is totally different than other pain situation. For example, you have the foot pain, knee pain, and they give you pain medication. They tell, “Don’t take until your pain level up to four or five.”
Dr. Lowenstein: Sure.
Dr. Ansari: The headache is exactly opposite. You take sooner. As soon as you feel migraine coming, you take it.
Dr. Lowenstein: So, basically, in the aura phase, if-
Dr. Ansari: If they have aura, which most of the patient does not have aura. But as soon as they feel headache is coming, then the level of headache is one or two, you take your headache medication. That’s why probably we don’t call headache head pain, because headache. Everywhere else we call it pain, but in the head we call headache. That’s why we do not use the pain medication for headache or we do not like to use pain medication for headache. We would like to use headache medication for migraine headache. So, abortive treatment is need for all of the migraine patient. Any patient with migraine needs to have abortive treatment, period.
Dr. Lowenstein: Okay.
Dr. Ansari: But preventive treatment or prophylactic, which is the daily medication, is for some percentage of the patients. Who is that percentage? The people who get more than certain number of the headache per month. The guideline that we has, it say if patient with migraine get more than five attack per month, which mean more than one per week, that patient needs to be on preventive treatment. We also use some other tools when we decide about the preventive. There is a lot of headache and migraine questionnaire which is kind of measurement tool. One of them is called MIDAS, one of them called HIT-6. That’s also important to decide if patient needs to be on preventive. If it scores higher, that mean headache affect patients life more, and that patient needs preventive. But general concept, more than one per week you need preventive treatment. That mean if patient with migraine using their abortive treatment more than one time per week, that patient needs to be on preventive treatment.
Dr. Ansari: So, let’s go back to the abortive treatment. Abortive treatment for migraine could be some simple, analgesics, right? Tylenol, acetaminophen, ibuprofen, naproxen, diclofenac. These are the medication, simple analgesics. Some of them are prescription like diclofenac, some of them is over the counter like ibuprofen. If patient migraine is not frequent enough and response to these simple analgesics, that’s fine, you have the patient taking three days per month of ibuprofen or Tylenol, and that works. That’s fine.
Dr. Lowenstein: That’s fine.
Dr. Ansari: But if the patient taking more than one per week, two, then three, that patient needs to be first of all given migraine as needed or abortive treatment, plus needs to talk about the preventive treatment. That’s why this over the counter medication sometime become a little basically confusing, because patient cannot count of course how many they take per week or per month, and that cause a lot of issue. Some of the over the counter medication is very easy to cause what we call the rebound headache. Those are combined analgesics like Excedrin. Excedrin is the medication that I personally do not use my patient take it because they don’t have any count how much they are taking and it’s very easy to overuse Excedrin without even knowing it.
Dr. Lowenstein: Okay. Yeah, you mentioned that on our last podcast as well.
Dr. Ansari: Yes, exactly. That is very, very important to make sure if the patient taking over the counter, have limitation. So, we have the simple analgesics. But when come to the prescription, the gold standout treatment for migraine abortive is triptan medication. The Sumatriptan, which is the oldest triptan, and we have since 1991 in the market. After that, there is six other triptan came to the market, Rizatriptan, Maxalt, for example, is the common one, and Eletriptran Relpax, Zolmitriptan Zomig, and Naratriptan Amerge, and Frovatriptan, which is Frova. These are the other triptan that we have in the market and currently FDA approved for migraine.
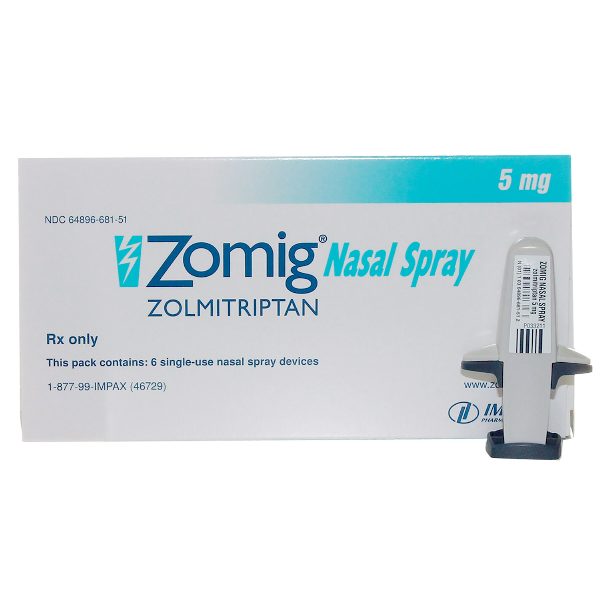
Dr. Lowenstein: And Imitrex is the Sumatriptan, right?
Dr. Ansari: Imitrex is Sumatriptan, yes.
Dr. Lowenstein: Yeah, okay.
Dr. Ansari: The oldest one, basically. All of the triptan come in the oral form, and some of them have injectable and also nasal spray format. Some of them also have the melting tablet like Maxalt makes melting tablet for. These are gold standard treatment for migraine abortive. Basically then we teach the resident, and let’s just say all migraine patient should have triptan as their treatment plan. So, rather than having over the counter or anything, use triptan when you’re having migraine rather than take with pain pill like ibuprofen, take migraine pill, which is Imitrex or Maxalt or one of these triptan medication. So, that’s important that all my migraine patient ask their physician to get the prescription for triptan. Yes, there is a small percentage that cannot take triptan, and that’s [inaudible 00:16:00], and that’s in the patient who had the cardiac disease like coronary artery, not the valve. This is not a [inaudible 00:16:09] problem. No, just the coronary disease, or the patient who had stroke, which fortunately this is very minority of our patient. Most of the migraine patient are in younger side and usually do not have heart attack or stroke. triptan in all of the migraine patient almost there is a clear contraindication.
Dr. Lowenstein: Can I just ask a couple quick questions? We know that we’re treating migraines basically with side effects of medications that are originally brought to market for other things. What other things were triptans used for before we realized that they were helpful for some migraine patients?
Dr. Ansari: Yeah, no, triptan actually wasn’t. triptan made for migraine.
Dr. Lowenstein: Oh, triptan were made for migraine?
Dr. Ansari: Yes, purely for migraine. Those are, we were talking those are preventive treatment that made for something else, and we are going to talk about that. For migraine treatment, triptan, basically that’s why. They have two evolution in migraine world. One is in ’90s, one is last year with the CGRP. We had abortive treatment, particularly for migraine, but we didn’t have-
Dr. Lowenstein: A preventative.
Dr. Ansari: … preventive treatment, particularly for migraine.
Dr. Lowenstein: Got it, okay. Then my other question is, I have a patient who I fixed the other day, I operated on, but prior to coming to me, they had been told that they could only take their triptan one time a week. This was from a rather prominent neurologist in Denver and she had said that you can only take the triptan one time a week until one of their biggest complaints was you had to pick and choose which migraine that week they wanted to treat with triptan. Can you overuse triptan? What are the risks with that?
Dr. Ansari: Yes. Actually, that one my next basically discussion about how much of the abortive treatment we can take. Since you brought it, let’s go through that part. Abortive treatment, or as needed treatment, as you can tell by the name, those are as needed. You cannot take all the time, because another thing when I see the patient and I’m giving the example of Excedrin patient come and say, “I’m taking Excedrin for prevent. No, Excedrin is not preventive, that is abortive, as needed. We cannot take any abortive treatment more than certain days per month. That certain days per month is different for each class of the medication. The safest class in term of not causing rebound headache or medication overuse headache is non steroidal medication, instead ibuprofen and naproxen class. There’s one medication in that class called a diclofenac potassium. Diclofenac come in two different salts, sodium and potassium. Diclofenac when on potassium actually has the highest evidence within that class of the medication, and that’s why the powder form of the diclofenac potassium called Cambia, which is a brand name, is FDA approved for migraine.
Dr. Ansari: Basically, it is the only FDA approved non steroidal anti inflammatory drug which approved for migraine. These class of medication up to 15 or even some of our colleague, and including me, I think up to 20 days per month it’s safe to take instead for migraine. Then in term of the abortive treatment, triptans, triptan it’s safe up to 10 days per month. So, a little over two per week. One per week is not great. Two, but 10 days per month, up to 10 days a month, triptan won’t cause a rebound headache.
Dr. Lowenstein: And that’s the concern is rebound? It’s not-
Dr. Ansari: Yes.
Dr. Lowenstein: Because I’ve read things about triptans in particular, that there was some concerns about whether or not they can cause stroke or other secondary effects.
Dr. Ansari: No, no. Stroke and heart attack, that’s why if the patient have a stroke or heart attack they cannot use triptan, but the chance that these cause a stroke and heart attack is not usually concern in somebody who’s healthy, doesn’t have cardiovascular disease or doesn’t have any heart problem or plug, otosclerosis disease or something, which most of our patient do not. One thing that we know is triptan is very, very underused or under utilized in United States. So, in one of the literature that I was reading, about 25, 30% of the patient with migraine they are prescribing triptan, while over 95% should have triptan. So, we have a big gap, and that’s because of all of these information that probably is online available. That’s why probably.But triptan is gold standard, as I mention. On this, there is the clear contraindication needs to be given for all of the migraine patients.
Dr. Lowenstein: Okay.
Dr. Ansari: Most of the patient that at least I see, they need both. They need both [Ensay 00:21:47] and triptan. Why? Because they have more than 15 or 20 days per month, or if they are going to take 10 days per month of triptan, what are they going to do rest of the month? Right? That’s why they need more than just triptan. For abortive treatment for migraine, we use two different strategy. One is called stepwise strategy, and the other one called attack specific strategy. What does that mean? The stepwise strategy, I tell my patient, “Okay, you’re getting headache. Take your Ensay, Naproxen, or diclofenac or Cambia, one of these [inaudible 00:22:26] at the onset of the headache and wait two hour. In two hour, 40, 50% of the time if you take early, the headache goes away and you don’t need anything. If that didn’t go away, then you can get your triptan. That’s called stepwise.
Dr. Lowenstein: Okay.
Dr. Ansari: The other one is the attack specific. This is something that patient needs to realize in which attack take which one. The patient can tell you after awhile when you talk to them, they really realize which attack is really bad, which one is less, and for milder one they use the Ensay, for the more severe one they use triptan one. They basically pick based on the attack which one they need to use. The other thing, two main thing that we do to increase our abortive basically approach and abortive treatment, one is in some patient, we need to give non oral triptan as a backup. Either self injection or nasal spray. Why? Because sometime patient take the triptan and pain doesn’t go away and they want to go out, they want to do some activities. So, for those patient we use the non oral triptan. Or another big indication for non oral triptan is for the patient with migraine who has wake up migraine. So, when they wake up with migraine, they are behind in the cycle of the migraine, so that when you are awake, we can, what? Take the medication as soon as we feel. Right?
Dr. Ansari: But when you sleep, you don’t know when your migraine started. It probably start four hours ago and now you are waking up. You are already in the end of your migraine or the peak of your migraine cycle. For those patient we use non oral treatment, and that’s why a lot of my patient I prescribe non oral, and that’s as a rescue. That’s a medication, I tell to my patient that’s a medication that keep you away from emergency room. So, we need that in most of the patient. The other strategy that we do to maximize the effect of abortive treatment is using some of this anti nausea medication, anti emetic. We had a lot of nausea medication, and few of them is shown to be very helpful in migraine. One of them is the metoclopramide, or reglan, and the other one is Prochlorpemazine or Compazine. These two has the highest evidence, and even there is evidence that this two nausea medication directly can decrease and hurt the migraine pain. There is a pharmacologic reason for that we can talk in a separate discussion.
Dr. Ansari: But these are directly… but at the least, these medication have two benefit for sure if you use with your abortive treatment, with your Ensay or with triptan. Number one, they will decrease the nausea. The nausea in some of the migraine patient is really bothersome. It sometime can be worse than headache. Second one what this medication does, and specifically metoclopramide, they increase their GI motility. We know that in the migraine, GI system become a little lazy during migraine attack. That means stomach and the bowel doesn’t move as good. When you don’t have that [inaudible 00:25:56] or that movement of the stomach, the medication does not absorb well. So, we’re using metoclopramide, you’re increasing that GI motility and that make the medication that you’re using with it like naproxen or [inaudible 00:26:13] or triptan absorb faster and work quicker. That is really important. A lot of people forget this. But I always use anti emetic in my patient with migraine to use with their ensay or to use with their triptan. That really, really helps to medication act faster and works better, plus help the nausea.
Dr. Ansari: This is in term of the treatment, abortive treatment of the triptan and non steroidal. There is other class of the migraine abortive treatment also available. One of the classes is ergot, which is one of the oldest migraine treatment, and actually at some point they used for prophylactic for a few years, but because of the side effect that they have, they removed it. But for abortive treatment, they’re still using. Ergot come in two different form. It used to come in two different formulation. It’s an injection and also in the nasal spray. However, since last two years, almost, we have the oral ergot, which called Ergomar. That is also available. Now we have the oral, we have nasal spray and injection ergot available. Those are different class of the medication, [inaudible 00:27:40] and triptan. But one thing that’s important, patient who are taking ergot, they cannot take triptan within 24 hour of taking ergot. They have interaction-
Dr. Lowenstein: One or the other.
Dr. Ansari: … with triptan. Yes, one or other. 24 hour interval between we comment. These are the basically three main class that they have. They used to have their very, very good migraine medication called Midrin, which is the combination of Tylenol with the component called [Oslometipton O00:00:28:14] as one of the oldest migraine medication, even before FDA started regulating. Unfortunately, the last two months it’s not available. I heard the company going to make it under other name and probably bring to market with much higher price. But that was very good migraine abortive treatments that we had. These are basically what we have in terms of the abortive treatment. The other thing about the abortive, there is a true class of the medication that some people use for migraine, and I do never, and I do not think any headache doctor use these two classes. One of those are opioid medication and including Tremetol, because a lot of times I see some physicians say Tremetol is the non opioid or recall period or something, which it’s not. Tremetol is opioid, synthetic opioid.
Dr. Ansari: The other class which is really, really strange is the Torbutrol, containing analgesics, fioricet and fiorinal. These are medication that, and fioricet and fiorinal is a medication that is never, ever even made for migraine and never ever approved for migraine, but probably that is the number one prescription for migraine by general physician, PCPs. That is a very, very big problem. Actually in the last article that I read, it said 34% in the USA use torbutrol or opioid for migraine.
Dr. Lowenstein: Really?
Dr. Ansari: That is huge number.
Dr. Lowenstein: We can do like four different podcasts just based on discussing opioids, but on the other hand I’ve seen so many people who are going to have this visceral response right here and say, “Okay, well I’ve tried the triptans and they don’t work, so I need my opioids.” There’s reasonable argument on both sides of that situation, but it’s unfortunate that not all medications are going to work for all different people, but you have to look at the bad with the good, which opioids has a lot of associated issues with it, but like I said, you and I should probably have another podcast where we’re just talking about opioids and fioricet.
Dr. Ansari: Opioids and fioricet. Fioricet is actually the biggest problem because your audience probably it’s good to know that fioricet actually is out of the market in the entire world except United States, which is very strange. This is a bit strange.
Dr. Lowenstein: You’ve got to love our FDA.
Dr. Ansari: and not do anything. But all over the world, you look years ago they removed it from the market because of a lot of issue that are happening with fioricet, and I see on my daily practice. But just simple thing about this fioricet and opioid, we are going to talk about anti CGRP treatment, right? There are three anti CGRP which we are going to talk about that, and there’s a clinical trial design to approve. Right? I mean, all of these three CGRP, the people with migraine who are taking opioid or tortubtrol excluded from the study.
Dr. Lowenstein: Okay, yeah. Yeah.
Dr. Ansari: So, that mean that you are taking that, the chance that you respond for any medication is very low.
Dr. Lowenstein: Right.
Dr. Ansari: This is basically abortive treatment. Any question in abortive treatment in particularly before we jump to the preventive?
Dr. Lowenstein: No. I mean, the only thing I would say is, again, I think we just have to acknowledge that not everything works for everybody. That’s why there are headache specialists who have a lot of, as we say, arrows in the quiver to try a lot of different things. Then at the end of the day, if medications don’t work, then that’s when people end up at my office for surgery. But yeah, I hope all of these issues, what we’re talking about is very educational for people to understand why you would progress through different things before giving up on meds. Anyway, let’s talk about preventatives.
Dr. Ansari: Yes. Preventive, again, indication is if patient with migraine had more than one attack per week or five per month, that patient require to be on preventive. This is the simplest explanation, but again, we have different tool also. So, now same patient needs to be on preventive treatment. What is the best preventive treatment? The answer is we do not have the best preventive. Best preventive is based on the patient. Each patient is different. We cannot look two patients exactly the same and use the same medication. But in general, we have three class of what we call the traditional migraine preventive treatment. Number one is antidepressant or anti anxiety medication. Number two is anti hypertensive blood pressure medication, and number three is anti epileptic or seizure medication. As you can tell and we briefly discussed at the beginning, none of these three class of medication is made for migraine, but study and trial show that some of those work for migraine. That doesn’t mean all of the anti blood pressure medication will work. It doesn’t mean all of the seizure medication, just the one that have a study and shown we use those.
Dr. Ansari: Although we might use the other one as a off label, but that would be totally off label or anecdotal, so that’s why we need to stick with the one that has FDA approval and has enough study to have evidence A or evidence B at least for treatment of the migraine. In term of the first class, which is anti depressant medication, the oldest one that they use is amitriptyline, or Elavil is the brand name. It’s one of the good basically anti depressants. We use with lower dose. One thing also that is important, the dose that we use for migraine is way lower than the dose that we use to explore the pressure. For example, in amitriptyline, we use something between 25 to 50. So, there is a medication which is cousin of the amitriptyline called nortriptyline or Pamelor that’s another medication from the exact same class. There is a medication called protriptyline or Vivactil from that class. So, there’s three medication in that class, but amitriptyline has the highest evidence.
Dr. Ansari: Then we have the newer anti depressant, and the one that had higher evidence is a medication called venlafaxine or Effexor. Although there is a, again, cousin of Effexor that’s called Desvenlafaxine or Pristiq. I like that a little better in term of side effect, but it’s almost impossible to get approval to the insurance. Basically these is two main anti depressants, amitriptyline or venlafaxine. Then we have the anti hypertensive or blood pressure medication. Beta blocker has the highest evidence in the patient in divided prevention, propranolol, nadolol, timolol, and metoprolol. This is four beta blocker that we use the most. After beta blocker, we have calcium blocker like Verapamil, and also the medication called Flunarizine, which we don’t have in the US, but Mexico and Canada have, and that’s why I have a lot of patient on that medication. Also, some of these what we call [inaudible 00:36:44] related anti hypertensive medication like Lisinopril or particularly Candesartan has some anecdotal evidence for migraine prevention. This is blood pressure.
Dr. Ansari: The third class is the seizure medication. The two medication in this class has FDA approval. One is topiramate or Topamax, and the other one is Depakote, which is valproic acid. One important, very important, actually, factor in this kind of preventive is using the correct dose or target dose. If somebody, I see this all the time, patient come and say, “I tried all of these.” When you look at their record it say, okay, patient tried amitriptyline 10 milligram, so I’m not expecting that anybody in 10 milligram will have a particular response. I tried it and, look, okay, I saw 20 milligram of propranolol. Nothing. It was basically you didn’t take anything. But that’s happened a lot. I understand why, because titration of this medication is not easy. So, when you put somebody on propranolol and you want to go to the target dose which is minimum 80 milligram, they use between 80 to 120 milligram propranolol. If you start somebody in 80 milligram of propranolol, that patient will take one or two dose and they will stop and done because of side effect. You need to titrate this medication every week, and that’s not easy, again, with the busy practice that all of the physician has. Who is going to see the patient every week or two week to titrate the medication?
Dr. Lowenstein: Sure.
Dr. Ansari: So, that’s very difficult. The same thing with Topamax. Topamax target dose is 100 milligram, but if you give somebody 100 milligram Topamax today, you won’t see that patient tomorrow. Probably those are horrible side effects, so that is the problem. The titration is the biggest problem. Slow titration, then you need to give time to the patient to basically become effective. The other important thing about the preventive treatment, because these are daily medication, of course they will have side effect. Right? You’re taking daily medication and each daily medication might have side effect. Some of them has more, some of them less, but also some patient might have a lot side effect to other medication, to medication X, but not to the Y, and vice versa.
Dr. Lowenstein: Even within the same class?
Dr. Ansari: Yes, exactly.
Dr. Lowenstein: Right.
Dr. Ansari: That is very important to discuss with the patient about the side effect and also look at the patient’s other comorbidities. For example, if patient has asthma, bad asthma, we cannot use propranolol. You are going to give the patient asthma attack. If the patient have the kidney stone or history of kidney stone, if you give Topamax, patient will have another kidney stone. I saw the patient just two months ago, this poor guy had nine surgery for kidney stone and he was in Topamax. Because of Topamax, nine time lithotripsy, and this is horrible.
Dr. Lowenstein: Wow.
Dr. Ansari: You need to ask all of these, and that’s not easy. Or if the patient is really overweight or obese, using amitriptyline is not good idea because you are going to give more weight gain. The same thing with Depakote, because weight gain and also hair loss, that’s why it’s not even possible in most of my patients. Most of my patient is female within 20 to 40, and the last thing that I want to tell my patient that I’m going to give a medication that make you fat and bald.
Dr. Lowenstein: Yeah.
Dr. Ansari: Right?
Dr. Lowenstein: Yeah, right.
Dr. Ansari: Right? So, no one can use that. That is that side effect is important. So, when you prescribe the preventive, they need to know the side effect very well, otherwise that will be a problem and the treatment won’t be successful. This is probably the main reason that medical treatment has not been as good for migraine because of the side effect.
Dr. Lowenstein: And there can be side effects as well for triptans, correct?
Dr. Ansari: Yes.
Dr. Lowenstein: A lot of people-
Dr. Ansari: But that’s abortive. The thing with abortive, even if it’s side effect, done, but preventive is daily. You have to take every day and decide if it’s not going to anywhere.
Dr. Lowenstein: Yeah, yeah. But I’ve had people who’ve told me that they didn’t like triptans because it wiped them out and it makes them really, really tired.
Dr. Ansari: But even side effect of the triptan which happen 10 to 15% of the patient called triptan sensation, again, we can talk about that.
Dr. Lowenstein: I get that, yeah.
Dr. Ansari: That doesn’t mean it happen with all of the triptan. If the patient have triptan sensation, which is feeling of the chest pain or throat swelling, those are the side effect that the patient get, with sumatriptan or Imitrex, you still can use other triptans. Some of the triptan we call it gentle triptan, so we use those. But again, that’s separate lecture that we can give. But we shouldn’t give up on the triptan that easy. Triptan is really, really good medication for migraine. This is three class of the preventive. Then we have Botox, which now is one of the oldest technique or oldest treatment that we have for migraine for last 10, 15 years even we are using it.
Dr. Ansari: One thing about the Botox that people need to know, it’s only approved for chronic migraines. Chronic migraine mean patient had 15 or more headache per month. So, the patient who are not chronic, Botox is not even FDA approved, although a lot of our colleague might use it, but it’s basically off label and it’s not FDA labeled to use it. That is very good treatment that we have. We still use it. I don’t remember the day that I do not have Botox injection in my office, so basically it’s every day. We use with a different technique. I use a little different than what is most of the neurologist does, because I actually learned Botox from non neurologist when I started it.
Dr. Lowenstein: Right.
Dr. Ansari: But that is very, very good treatment that we have.
Dr. Lowenstein: And you can do a whole nother podcast on that. I cover that a lot on my website headachesurgery.com. But yeah, one of the issues that I have is that I see patients who have had Botox and it didn’t work, and people come in with occipital problems and they had… was it 33 injections of the normal?
Dr. Ansari: 31.
Dr. Lowenstein: 31 injections from the FDA. Seems like honestly a waste of a lot of Botox in parts of the head that are not affected. But yeah, we’ll have another episode on this.
Dr. Ansari: I agree, actually. There was a meeting called toxin meeting. It was a very good meeting, actually, that all of the specialty that I use Botox, they come to that meeting. I attended that meeting and I had the lecture that was in Spain 2017. We were talking, and actually one of the speaker was the ear, nose, throat physician. They was taking about the Botox. During his presentation, he actually make a joke that neurologists overuse the Botox. I agree. We overuse. We really don’t need that many injection. But again-
Dr. Lowenstein: But anyway, that’s yet another podcast to listen for on future episodes. But okay, let’s move on.
Dr. Ansari: Move on, okay. Then in term of the newer preventive treatment which really, really change the way that we practice since last year is this new anti CGRP. Just a quick description about what is CGRP. CGRP is the neural transmitter, basically chemical in the brain, calcitonin gene-related peptide. That is the chemical in the brain that cause inflammation. Inflammation in the brain which is a neural inflammation is the key component of creating the headache. Now when we talk about the migraine, we call migraine is the neuro inflammatory disease. The CGRP is a key player in this neuro inflammatory. That is in term of what is CGRP. Now, what happen if we decrease the CGRP, because studies show that in the patient with migraine, CGRP level increase. So, if you can decrease the level of CGRP, it will be helpful for a migraine. This was the theory, although it wasn’t this easy. Now it’s very easy. It seems very easy, but if you look at the discovery of CGRP, CGRP actually discovered back in 1982 here in University of California, San Diego, where they were then working, by two pharmacy PhD doctorate basically physicians. They discovered it at 1982.
Dr. Ansari: Then they didn’t know what exactly it does until ’90, which Dr. Edvinsson, the current president of International Headache Society, he for the first time explained that CGRP is a player in migraine, and then ’91 when Dr. Goadsby continued that discussion and they confirmed, yes, CGRP. So, 1991, we know that the CGRP is a key player, or at least one of the key player for migraine, but we didn’t have anything until 2018, so it take 28 years until we know what it is until the medication that works on that. That mean a lot of work done until then. Now we have three medication which basically works in the CGRP and antagonize the CGRP, that’s called anti CGRP, monoclonal and [tibadi 00:47:15]. These are either humanized or fully human monoclonal and tibadi. First one made by Amgen and launched by Amgen Novartis back in May of 2018, that’s called Aimovig. There is actually TV commercials, and some of your audience might see that.
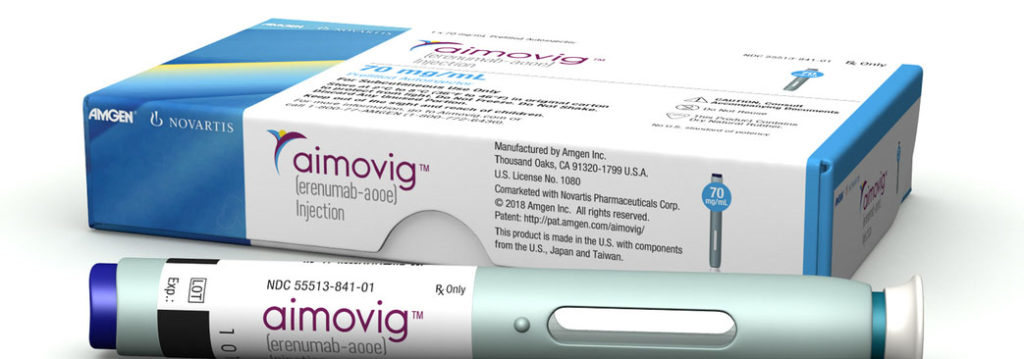
Dr. Ansari: Then there is two other one come within a week from each other in September of 2018. One of them is AJOVY by Teva Pharmaceutical, and the other one is Emgality by Eli Lilly Pharmaceutical. Now we have three available. There is not much difference. The big difference is between Aimovig and the other two. Aimovig basically blocked their receptor of CGRP, so any chemical in the brain needs some receptor go and click and start working. What Aimovig does is block the basically receptor, and the other two AJOVY and Emgality, they are blocking the molecule itself. They directly block the CGRP. The beauty of these class of the medication is once a month rather than every day, and actually one of them, AJOVY, you can do quarterly rather than once a month. Three injection every three months. But all three stand out treatment is one every month.
Dr. Ansari: Subcu injection, they come with the oral injector or prefilled syringe. It’s very easy to use. They do not even go to the lever to metabolize through the lever. That mean there is no interaction with the other medication that patient might take, and doesn’t do anything with the patient’s other underlying disease you have. Asthma, kidney stone, whatever you have, there’s no problem because they won’t have any problem with any of other system, because that’s go subcu to the blood and then through the blood metabolize to the system, where phagocytosis is basically what they remove their molecule from their body.
Dr. Ansari: This is the new three class that we have and kind of changed stigma of the migraine, changed the practice because now we have something that’s specifically made for migraine. As I mentioned, the other three classes or four classes in Botox, which we’re using, is not made for migraine. Botox was basically a new drug for awhile, plastic surgeon, right?
Dr. Lowenstein: Yeah. Then for aesthetics.
Dr. Ansari: Exactly.
Dr. Lowenstein: But now people use it in muscle spasms all over the body.
Dr. Ansari: For everything. Using for hyperhidrosis and everything.
Dr. Lowenstein: Right.
Dr. Ansari: Yeah. Basically these are the first ever migraine preventive treatment. Any question in CGRP?
Dr. Lowenstein: That’s a trick question unto itself. I’m sure we could talk about CGRP also for quite some time. I guess my experience is skewed because the people that I see are the people who fail everything else. Right? You try this medication, that medication, and none of them work or the side effects don’t work for them for a multitude of reasons. Then they end up in my office for nerve decompression surgery. Can you briefly discuss why X, Y or Z would not work for a given patient, or are we still trying to figure that out?
Dr. Ansari: You are talking about the traditional treatment, or…
Dr. Lowenstein: Well, I guess you can, since there are no, except for the CGRP blockers, the preventatives have never been specific for migraines, and so you could have certainly people who just don’t tolerate the low heart rate associated with a beta blocker or the exhaustion that’s associated with antidepressants, and certainly there are people who I’ve had that have tired triptans and they say they don’t work for them. There are certainly lots of reasons Botox could not work, and primarily again, I think a lot of people who don’t necessarily know how to properly inject Botox for migraines are part of the issue, because I’ve seen a lot of people who just are getting injections in the wrong spot. Then there’s CGRP drugs that I think, from what I see, work for some people but don’t seem to work for others. I guess would I be correct in saying that you progress through these different types of medications as needed? If one works, that’s great, if one doesn’t work, then you move onto the next one, and then at some point if medications don’t work, then you move onto other modalities?
Dr. Ansari: Yes, exactly. In term of the traditional treatment why it failed, one of the main reason is because, as we discussed, these are not made for migraines, so you don’t expect that something that’s not made for that condition helps for all of the patients. Right? Second of all, the side effect. A lot of people do not tolerate the side effect in the dose that they need to be in. That is probably even more important than that. If all of the patient can tolerate the traditional preventive with their target dose, we certainly will have higher side response rate. But again, the side effect is the problem. In term of the CGRP also, we are not expecting to be 100%, because although we know CGRP is a key player in the neurogenic inflammation, but it is not the only player. We have other neural transmitter that play a role. You have the different type of the migraine. Migraine is a genetic disorder, we discussed in our first podcast, I believe. A migraine is a complex genetic neurological disorder. That mean not all of the patient had the similar gene.
Dr. Ansari: Yes, in a majority of the patients, CGRP seems to be the key player, and that’s why the response rate is really, really high if you’re using the correct patient. I really see very few failure, and actually the people that fail the CGRP and send it to me, even you go and dig and they have some other reason. For example, they are still taking opioids. If you take opioid, CGRP is not going to be effective. There is a pharmacologic reason for that, because opioid increase the CGRP, so you are increasing CGRP with opioid and you’re trying to be anti CGRP, so you’re wasting your time.
Dr. Lowenstein: Sure, okay. Interesting.
Dr. Ansari: That is the thing. But yeah, there definitely won’t be 100%. Again, we don’t have any cure for any disease that have genetic basis. Right? We cannot cure the diabetes, we cannot cure the hypertension. The migraine is like that. This is some gene is going on and we just can’t manage it better. But if there’s traditional treatment and more recently the CGRP fail, there is a lot of other options. We use a lot of procedures besides Botox for the migraine even for many years, and one of those procedure are nerve block. The nerve block is the lidocaine injection in the different nerve that we do. That’s very helpful. I have a patient that come every two weeks for a nerve block for last three years, because that patient had a single trigger point and she doesn’t want to take daily medication and that works. So, if that’s the case we do that. There is other basically modalities like devices.
Dr. Ansari: There is a lot of new devices that your audience might hear. These are neural stimulator devices that is in the market, and there’s three main neuro stimulator. One is for supraorbital nerve, which called Cefaly device. One of them is for the occipital, which call Spring TMS Device, and one of them for vagus nerve that called gammaCore. These are the three devices that available and approved for migraine treatment. In my experience, those are not very effective, or at least not very effective in the patient who failed a lot of other medication. Yeah, if you use in the firsthand patient, it probably will be helpful, but in firsthand patient, any other treatment will be helpful.
Dr. Lowenstein: Actually, we’ve had a pain specialist on the podcast as well, and he’s the kind of guy that would actually be putting those in, and he feels exactly the same way.
Dr. Ansari: That’s different. The pain specialist, actually the one that you did, I’m talking these are external stimulator. They basically-
Dr. Lowenstein: Oh, external simulator. Okay.
Dr. Ansari: Yeah. This device and patient does itself. The other one that is occipital stimulator of the place lead, that is actually, there’s a huge study done in male clinic years ago, and it showed that it failed and it’s never approved for migraine. In my experience also, the side effect and complication is way higher than basically possible or potential benefit.
Dr. Lowenstein: Got it.
Dr. Ansari: That’s why that’s st that I do not recommend. Between that placement of the occipital and your procedure which is occipital decompression, I don’t want to be biased, but definitely the occipital decompression has much… definitely safer, and also, in my opinion, much more effective.
Dr. Lowenstein: Great.
Dr. Ansari: Since we talk about this procedure which is your niche, basically, yes, the migraine trigger point, the activation surgery which invited by Dr. Guyuron back in first time actually explaining 2000, 2001. Since then he is doing that. That is one of the procedure that we do for some of our patients. The question which patient will be candidate for that and each patient is not, this is, I think, is one podcast that I would like to do because I want to give my opinion in that. We don’t have to do in the patient that fail everything. That’s my opinion. It’s very similar to other procedure that we have in the basically neurology world. We have the condition and trigeminal neurology, and that’s a condition that caused from compression of the blood vessel in the trigeminal nerve in the brain. When I see that patient in my clinic, I always recommend surgery first, because that’s kind of a cure.
Dr. Ansari: The same thing with the trigger point. I don’t wait until patient fail everything, because basically you want to waste three, four, five years of the patient’s life with being miserable and suffering while you know that this procedure which is relationship safe, right, we’ll talk about that hopefully in your podcast that you probably can tell about the complication and side effect, but if you compare this with this occipital stimulator which the pain doctor does, this is way safer and less side effect.
Dr. Lowenstein: Yeah. We’ll have to definitely do… I mean, in the next weeks to months I’ll probably do a podcast myself on what I do, which is this trigger point and nerve decompression surgery invented by Dr. Guyuron, who is a friend of both of ours and somebody that we both have a tremendous amount of respect for. But yes, I agree that our success rate and our safety profile is outstanding for that procedure. It just works, as we say. But again, a different podcast. Any other comments that you want to make about medications? Because the one thing that I’m taking away from this is how important it is to see somebody who really knows what they’re talking about, because you’ve got preventatives, you’ve got abortives, you’ve got the newest drugs, you’ve got all of these different side effect profiles and all of these different dosage profiles. It’s a lot of information. People ask me about medications all the time, and I defer to headache specialists because that’s not my world. So, I really think it’s important to make sure that patients are seeing people who are well versed in the specialty of headache.
Dr. Ansari: Exactly. Now you can actually refer to this podcast, because I think we discussed the classes, abortive. This is very important. One thing that I want your audience know the difference between preventive and abortive treatment and not using abortive treatment more than supposed to be, particularly over the counter medication. That will make the headache worse.
Dr. Lowenstein: Yeah. All right. Well, Dr. Ansari, again, thank you very, very much. I look forward to hopefully many more of these podcasts. I think today we’ve identified several other areas that we can talk about.
Dr. Ansari: Sure, sure. Exactly. Thank you very much again, and hopefully this is helpful for your audience and they can get some benefit and some education and information about the headache and migraine and treatment.
Dr. Lowenstein: Fantastic. Okay. Thanks everybody for listening, and we all look forward to hearing from Dr. Ansari again. There you go. Thanks very much.
Dr. Ansari: Thank you.
Dr. Lowenstein: Hey, everybody. This is Dr. Lowenstein once again, and I have two last things to ask of you. Firstly, the thing you can do for fellow headache sufferers is to please remember to subscribe and rate our podcast. More ratings and subscriptions that we get, the more visibility that we’ll get, and the more listeners will be able to find us, and the more help and information we’ll be able to provide the huge population of people who suffer from headache pain. Secondly, please remember that the treatment of headaches of all types is very individualized. The purpose of this podcast is not to give medical advise, so please use the information here on this podcast and elsewhere that you hear on the internet to broaden your knowledge, but consult with your physician before acting on any information that you hear on podcasts or see on YouTube, or read anywhere on the internet. I as a physician don’t necessarily endorse the opinions or practices of my guests, and if you have particular questions that you’d like to consult with me directly about, please call our headache surgery center. Our phone number is 8059699004, or you can email us at info@headachesurgery.myfastpic.com, and my staff will set up a consultation and we can discuss your specific case over the phone or in person. Our website is filled with information as well, and that is headachesurgery.com. Thanks and best wishes from all of us here at the Headache 360 podcast.

